EHR Integration - 7 Steps to Ensure Success

Whether your EHR implementation is expected to take six months or many years to install across all facilities, the key to a seamless Integration relies on the execution of these 7 critical steps. Failure of one of these steps can cost a health system millions of dollars and years of questionable data integrity.

1. It All Starts with a Great Plan
Accessing readiness and determining the best EHR vendor partner are the most critical factors to consider during planning. This partnership will affect all other decisions that are made from this point forward. Analyzing requirements and defining the goals and objectives for the enterprise are the first steps in planning for a successful and seamless EHR implementation. Once those goals are defined, an EHR vendor can be selected to achieve those goals within the determined timeframe. Developing an all-inclusive project plan that includes tasks, resources and milestones will determine if the timeframe is obtainable with current resource allocation or if outside help is required. The deliverables of this step are essential to maintain an on time and under budget seamless EHR implementation.
2. Understand the Current Health System’s Technological State.
By understanding and documenting the current technological state, you are better prepared to reach the required future state. The documentation of the current state technology along with a clear understanding of your EHR requirements will allow for a detailed gap analysis. This gap analysis is used to develop a detailed plan of specific tasks that are required to meet the desired level of technology in the timeframe allocated. That timeframe and number of tasks helps determine if the current resource pool can handle or if outside assistance is required. Three objective outcomes from this service include: documentation of current technology state, gap analysis, and recommendations based on our years of experience assisting other health systems throughout the nation with their EHR implementation.
3. Data Architecture and Workflow Analysis.
One key area that sometimes falls behind during an EHR implementation is the system design. Working with the existing and new ancillary vendors to collect all of the specifications is a critical step in the Implementation process. Having the expertise to validate specifications and perform the required data architecture analysis to create a data diagram or new data delivery structure is key to a seamless EHR integration. Along with a complete understanding of the data flow, the need for workflow analysis is essential to meeting the deadlines of the build and testing phases. Having the leaders in place to assist with department interviews that help analyze clinical and financial workflow, allows for future testing plans and build requirements. Documentation of these workflows via Visio diagrams are an exceptional output from this step of the implementation.
4. Configuration and Manipulation of Data.
It’s all about the data. No matter the EHR vendor software or the integration engine used at the site, the need to manipulate the format of the data is an essential step in the EHR implementation. Following the specifications from the design phase, the interface build is usually a very time consuming activity. However, by using the gap analysis and the documented data specifications, this process becomes a controlled activity. The time spent in earlier activities allows the programmers to perform heads down work and hit their deadlines.
During the design phase, determining what data is required and what data conversions are necessary is an important deliverable. Whether the data is being converted from an ancillary system being replaced or from an existing hospital computer system, the need for specialized resources to develop code to extract the data in the required format is essential. The use of internal resources sometimes helps with this process; however this can also limit the staff’s ability to come up to speed on the new EHR technology. A decision needs to be made up front whether to use external resources to focus on existing / legacy systems. Utilizing external resources will allow internal staff to focus on the new EHR implementation.
You may want to consider outsourcing your legacy support services and support agreements to allow internal staff to focus on the new EHR implementation. Keeping the focus on the new technology and removing the legacy dependencies helps staff transition to the new technology more proficiently and speedily. It also allows for a more controlled change management policy for your legacy systems.
5. Testing
This is usually the first area to be reduced when the project begins missing deadlines. Validation of the configuration and designed workflows through a series of functional, unit, mapped record and integrated testing phases are the only way to truly understand the go-live readiness position. A solid plan must be in place to bring together the appropriate resources and application workflows to develop highly effective health system specific integrated test scripts. When these integrated test scripts are combined with the integrated testing status reports, a very clear picture of readiness is available on a daily basis through each round of integrated testing.
6. Implementation – It’s All in the Delivery
Now that all the tasks are completed and the system build has been thoroughly tested, it’s time for the go-live. Scheduling resources for the go-live coverage is a huge undertaking, when considering the number of resources and hours of coverage. This is especially true when dealing with multi-facility health systems.
7. Support
Just when you thought the go-live was the last step, along comes the question of support. Once the go-live is complete and the decision is made to close down the command center, error resolution and user training continues. As much as one would like to believe that life goes back to normal after the go-live event, it is not always that simple. Allocating time for staff to continue the support of the Legacy systems and resolving issues of the new EHR is sometimes overwhelming. HCI has the ability to cost effectively support your legacy applications. Knowing that millions of dollars are invested in an EHR, we understand the importance of having staff focused on the new technology. We have experience working with a broad array of healthcare applications and can offer support to a legacy system that assures trouble-free operation for as long as it remains in service. We understand the importance of the technology investment, and to help ensure success, our resources will be experienced and fully certified in the legacy system as well as any new system being adopting. We’ll keep the legacy system running while you focus on the future. Seamless integration between disparate systems in a hospital and its network is one of the toughest challenges each health systems faces today. Through our innovative support program outlines below, HCI can help you meet these challenges head on by participating in the project planning, providing assessments, leading your project team or supplementing your staff at every stage of this journey.
A SMARTER APPROACH TO INTEGRATION & TESTING – HCI’S MONTHLY INTERFACE AND MONITORING PROGRAM
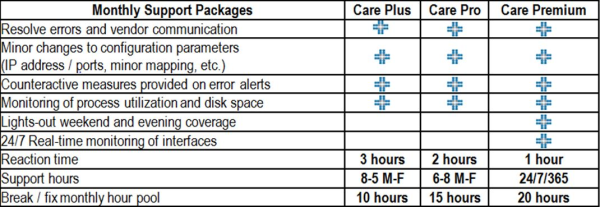
The HCI Group provides interface support and monitoring for your organization in a flexible and cost effective model designed to meet your complete departmental and budgetary needs. Our tiered monthly support programs provide:
The HCI Group, a world leader in healthcare IT consulting, is proud to be INC Magazine's 2013 fastest-growing healthcare company in the U.S. Our services include implementation and training of all EHR vendors as well as specialty service lines in optimization, clinical adoption, integration and testing, go-live, and advisory services, among others.
For more information on our integration and testing solutions, please contact our VP’s of Integration & Testing:
Mark Jackson: 904-337-6353, Mark.Jackson@thehcigroup.com
Scott Hassler: 517-819-5849, Scott.Hassler@thehcigroup.com
